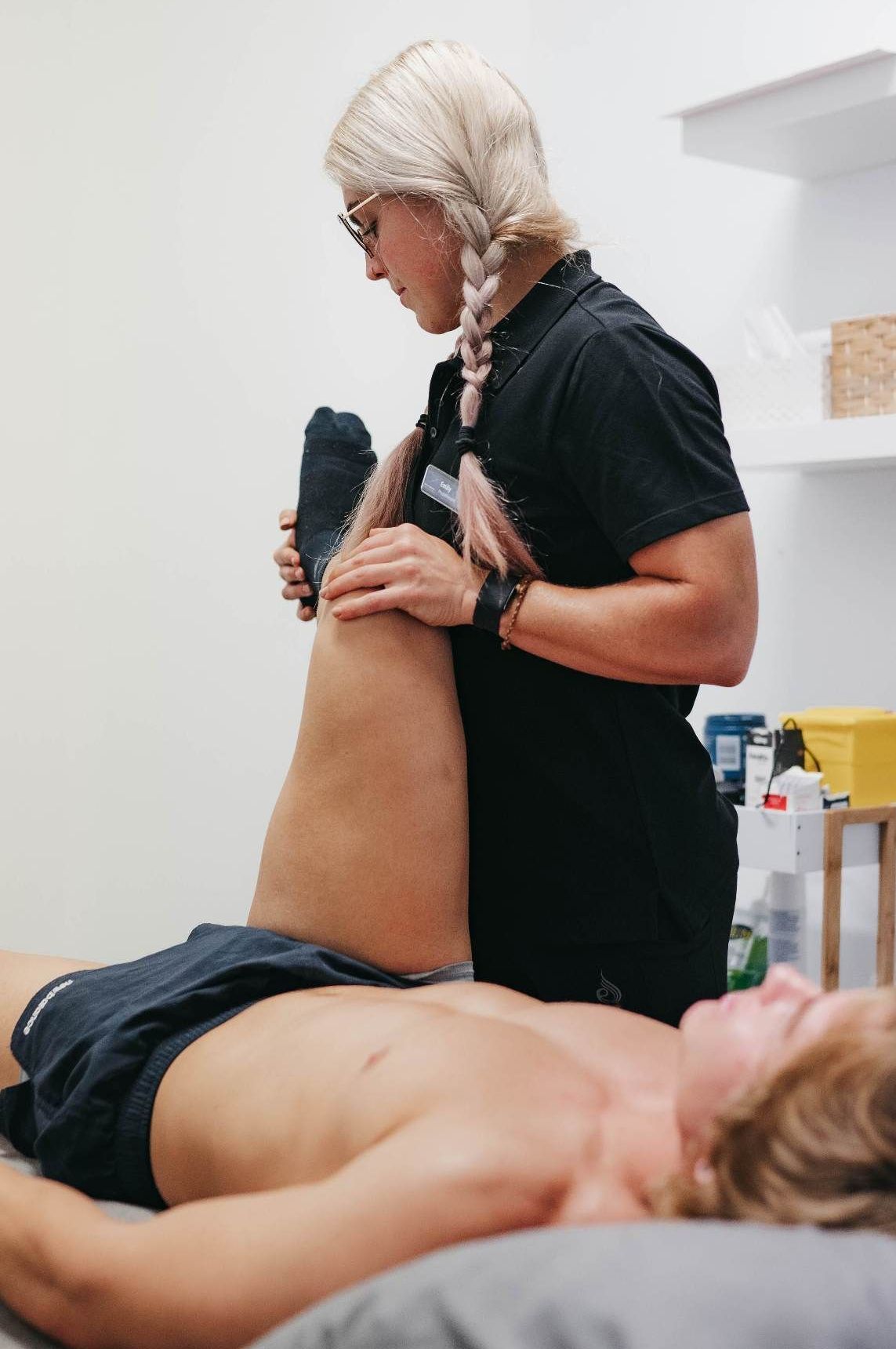
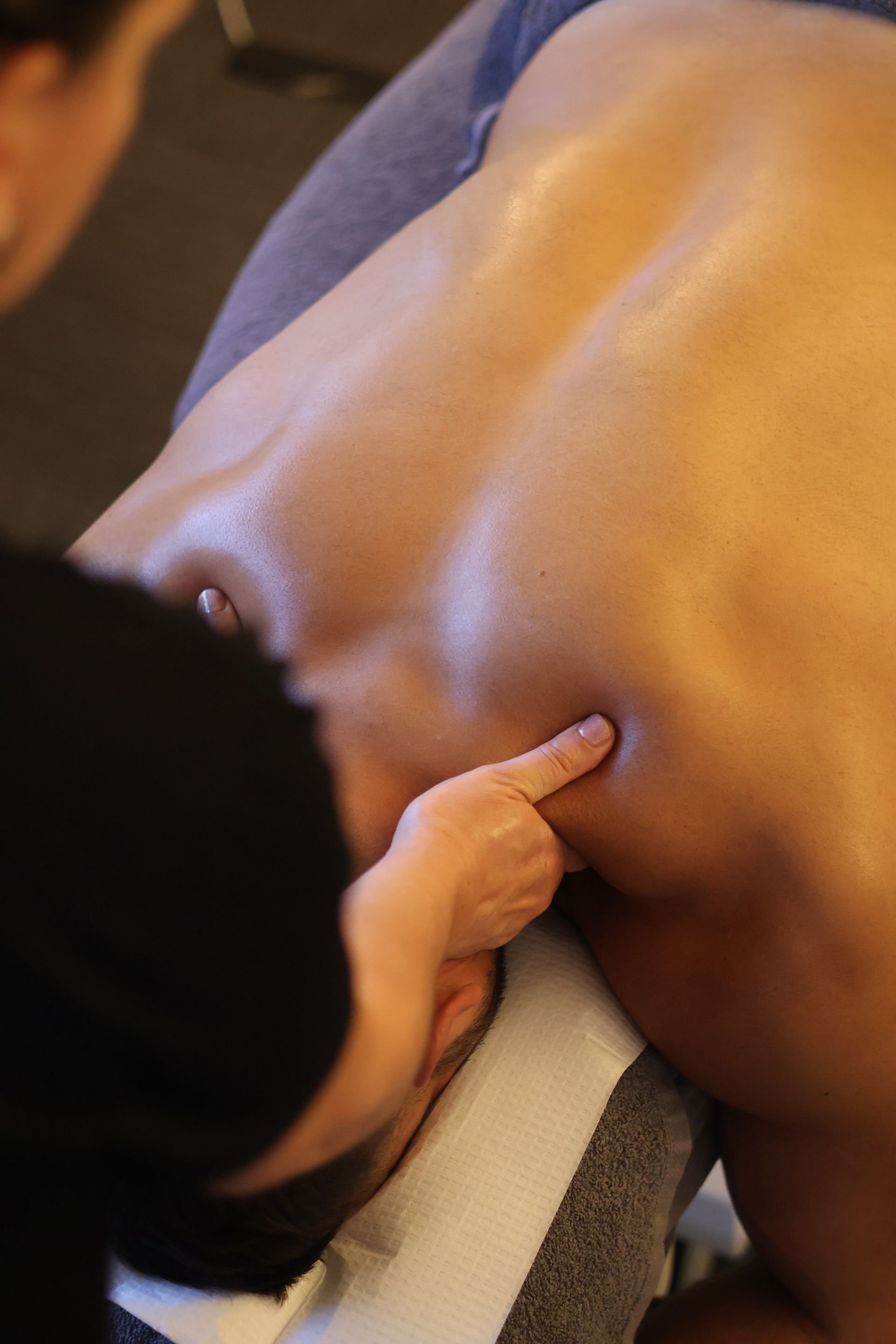
Your Home for Movement, Recovery & Wellness
Physio-led care, combined with massage, myotherapy, clinical exercise and recovery services to keep you feeling & performing at your best.
Welcome to Active Balance Physio & Wellness
We deliver high-quality, personalised physiotherapy, recovery and wellness services to both local clients and those from all over Adelaide, from our clinic in St Marys.
Our holistic approach combines expert hands-on care with clinical exercise and rehabilitation in a warm, inclusive space where every client feels valued.
Whether you’re local to St Marys or travelling from further afield, we’re here to help you move better, recover well, and feel your best.
Our Services
Learn more about our range of services below. We offer high-quality, personalised care with a holistic approach in a friendly and welcoming space.
Physiotherapy
Book an AppointmentRemedial Massage
Book an AppointmentRehab Gym
Book an AppointmentNot sure what’s right for you? Check out go-to guide here!
Otherwise, our friendly team is always happy to chat and guide you.
Get in touch with us
here.
We serve clients from across all of Adelaide — from the northern suburbs and eastern suburbs to the southern suburbs and Adelaide Hills. In our local area we are convenient for: Clovelly Park, Pasadena, Bedford Park, Edwardstown, Melrose Park, Daw Park, Panorama, Colonel Light Gardens, Clarence Gardens, Marion, Darlington, Mitchell Park, Tonsley, Bellevue Heights, Eden Hills, Ascot Park, Oaklands Park, Warradale and surrounding suburbs.
Why Our Clients Choose Us
Locally Owned & Operated
Deeply rooted in the local community, proudly supporting local sports clubs and not-for-profits.
Experienced, Highly Skilled Staff
Our clinicians regularly upskill through in-house training and external courses to deliver the best possible care.
Caring and Friendly Team
You’ll never be just a number here. We create a warm, welcoming space where every client feels genuinely valued.
Generous Appointment Times
Longer sessions so we can listen properly and treat you thoroughly — no rushing you through
Inclusive Environment
A safe space for everyone — gender-diverse, neurodiverse, and LGBTI+ clients are warmly welcomed.
Fully Equipped Gym
On-site gym with cardio, strength equipment, barbells, cable machines, and advanced performance testing.
Holistic Care
Multiple modalities plus a dedicated recovery room — our team works together for your best results.
Convenient
After-hours and weekend appointments to help fit around work, family, and real life.
Latest News
Get the latest news and advice from our team of experienced health professionals